Alzheimer’s disease is a form of dementia. It is a slowly progressive disease starting with mild memory loss and possibly leading to loss of the ability to hold a conversation and respond to daily activities. Alzheimer’s disease involves parts of the brain that control memory, thoughts, and language. Alzheimer’s can seriously reduce a person’s ability to carry out daily activities.
In 2020, as many as 5.8 million Americans were living with Alzheimer’s disease. Symptoms of the disease can first appear at age 60, and the risk increases with age.
Getting checked by your primary care provider can help determine if the symptoms are related to Alzheimer’s disease or more treatable conditions such as a vitamin deficiency. Early and accurate diagnosis also provides opportunities for you and your family to slow down the progression of the disease and plan for the future. Earlier diagnosis and intervention techniques are improving dramatically, and treatment options and sources of support can improve quality of life.
Stages of Alzheimer’s Disease
Alzheimer’s Disease is a slowly progressing, irreversible neurodegenerative brain disease with a very long preclinical phase (up to 20 years) and an average clinical duration of 8 to 10 years. The progression of Alzheimer’s disease is accompanied by changes to the brain that serve as biomarkers of the disease. Disease progression typically spans several stages. These stages include preclinical Alzheimer’s disease, mild cognitive impairment (MCI) due to Alzheimer’s disease, and Alzheimer’s disease dementia varying from mild to severe.
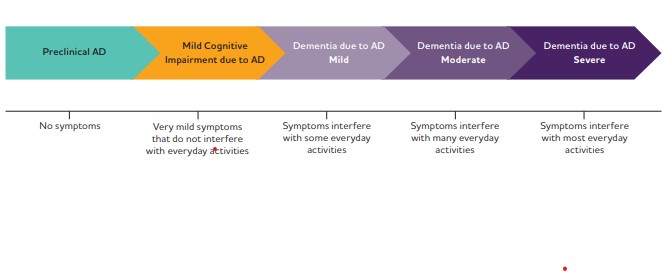
Symptoms depend on the stage of the disease
Early symptoms include:
- Memory loss
- Misplacing items
- Forgetting the names of places and objects
- Repeating themselves regularly, such as asking the same question several times
Middle-stage symptoms include:
- Obsessive, repetitive, or impulsive behavior
- Delusions (believing things that are untrue)
- Problems with speech or language (aphasia)
- Disturbed sleep
- Changes in mood, such as frequent mood swings, and depression.
- Difficulty in performing spatial tasks, such as judging distances
- Finding it hard to remember things
- Asking the same questions over and over
- Having trouble paying bills or solving simple math problems
- Getting lost
- Losing things or putting them in odd places
- Increasing confusion and disorientation
Later symptoms include:
- Difficulty in changing position or moving around without assistance
- Forgetting how to brush teeth or comb hair
- Gradual loss of speech
- Significant problems with short and long-term memory
- Being confused about time, people, or places
- Forgetting names of common things, such as a desk, house, or apple
- Wandering away from home
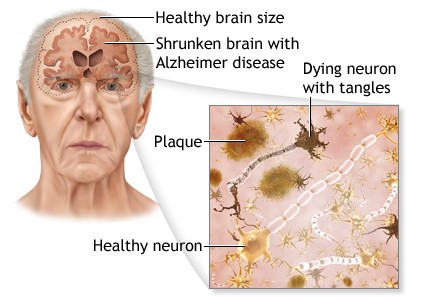
What Happens to the Brain in Alzheimer’s Disease?
The healthy human brain contains billions of neurons—specialized cells that process and transmits information via electrical and chemical signals. They send messages between different parts of the brain, and from the brain to organs and to the muscles of the body. Alzheimer’s disease disrupts this communication among neurons, resulting in loss of function and cell death.
Biological Processes in the Brain
- Most neurons have three basic parts: a cell body, multiple dendrites, and an axon.
- The cell body contains the nucleus, which houses the genetic blueprint that directs and regulates the cell’s activities.
- Dendrites are branch-like structures that extend from the cell body and collect information from other neurons.
- The axon is a cable-like structure at the end of the cell body opposite the dendrites and transmits messages to other neurons.
The function and survival of neurons depend on several key biological processes:
Communication. Neurons are constantly in touch with neighboring brain cells. When a neuron receives signals from other neurons, it generates an electrical charge that travels down the length of its axon and releases neurotransmitter chemicals across a tiny gap, called a synapse. Similar to a key fitting into a lock, each neurotransmitter molecule then binds to specific receptor sites on a dendrite of a nearby neuron. This process triggers chemical or electrical signals that either stimulate or inhibit activity in the neuron receiving the signal. Communication often occurs across networks of brain cells. In fact, scientists believe that in the brain’s communications network, one neuron may have as many as 7,000 or more synaptic connections with other neurons.

Metabolism. Metabolism—the breaking down of chemicals and nutrients within a cell—is critical to healthy brain cell function and survival. To perform this function, Brain cells require energy in the form of oxygen and glucose, which are supplied by blood circulating through the brain. The brain has one of the richest blood supplies of any organ and consumes up to 20 percent of the energy used by the human body. It is much higher than any other organ.
Repair, remodeling, and regeneration. Unlike many cells in the body, which are relatively short-lived, neurons have evolved to live a long time—more than 100 years in humans. To live for such a long time, neurons must constantly maintain and repair themselves. Neurons also continuously adjust, or “remodel,” their synaptic connections depending on how much stimulation they receive from other neurons. For example, Neurons may strengthen or weaken synaptic connections, or even break down connections with one group of neurons and build new connections with a different group. Adult brains may even generate new neurons—a process called neurogenesis. Remodeling of synaptic connections and neurogenesis is important for learning, memory, and possibly brain repair.
Neurons are a major player in the central nervous system, but other cell types are also key to healthy brain function. In fact, glial cells are by far the most numerous cells in the brain, outnumbering neurons by about 10 to 1. These cells, which come in various forms—such as microglia, astrocytes, and oligodendrocytes—surround and support the health and function of neurons. For example, microglia protect neurons from chemical and physical damage and are responsible for clearing cellular debris and foreign substances from the brain. To carry out these functions, glial cells often collaborate with blood vessels in the brain. Together, glial and blood vessel cells regulate the delicate balance within the brain to ensure its functions.
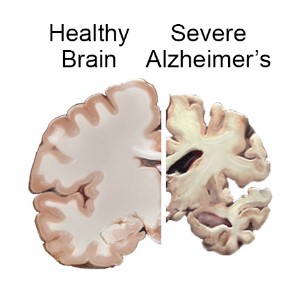
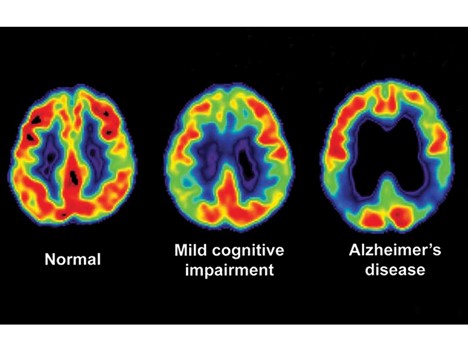
How Does Alzheimer’s Disease Affect the Brain?
The normal brain typically shrinks to some degree in healthy aging but, surprisingly, does not lose neurons in large numbers. In Alzheimer’s disease, however, the damage is widespread, as many neurons stop functioning, lose connections with other neurons, and die. Alzheimer’s disrupts processes vital to neurons and their networks, including metabolism, communication, and repair.
At first, Alzheimer’s disease typically destroys neurons and their connections in parts of the brain involved in memory, including the entorhinal cortex and hippocampus. It later affects areas in the cerebral cortex responsible for language, reasoning, and social behavior. Eventually, many other areas of the brain are damaged. Over time, a person with Alzheimer’s gradually loses the ability to live and function independently. Ultimately, the disease becomes fatal.
Role of Food/Vitamins in Alzheimer’s Disease?
Diet plays a significant role in introducing antioxidant and anti-inflammatory factors, shaping microbiomes, and treating digestive problems such as gluten sensitivity, which might decelerate inflammation and Alzheimer’s progression. The inflammatory events throughout an individual’s lifetime suggest the presence of a chronic inflammatory condition. The cumulative effects of this chronic inflammation may impact the different stages of Alzheimer’s Disease. Developing anti-inflammatory lifestyle habits may likely slow the progression or delay the onset of Alzheimer’s Disease. Health behavior interventions, such as proper dietary intake and supplements, may delay or slow the progression by 3 to 5 years. Educating the patient or caregiver on delaying Alzheimer’s Disease by early detection of the disease in combination with early intervention can act as an effective method to manage the disease and control the progression.
What can you do to prevent or slow down progression of Alzheimer’s Disease?
Changes in the brain can occur years before the first symptoms of Alzheimer’s appear. These early brain changes suggest a possible window of opportunity to prevent or delay dementia symptoms. Scientists are looking at many possible ways to do this, including drugs, lifestyle changes, and combinations of these interventions. Unlike other risk factors for Alzheimer’s that we can’t change, such as age and genetics; however, people can control lifestyle choices such as diet, exercise, and cognitive training.
What do we eat affects our brains? Eating a certain diet affects biological mechanisms, such as oxidative stress and inflammation, that underlie Alzheimer’s. Diet also works indirectly by affecting other Alzheimer’s risk factors, such as diabetes, obesity, and heart disease.
Not all studies have shown a link between eating well and a boost in cognition. Overall, the evidence suggests but does not prove, that following a Mediterranean or similar diet might help reduce the risk for Alzheimer’s dementia or slow cognitive decline.
Ingredients of the MIND Diet
The MIND diet focuses on plant-based foods linked to dementia prevention. It encourages eating from 10 healthy food groups:
Leafy green vegetables — minimum 1 serving/day
Other vegetables — minimum 1 serving/day
Berries– minimum 2 servings/week
Whole grains– minimum 3 servings/day
Fish — 1 serving/week
Poultry– 2 servings/week
Beans — 3 servings/week
Nuts — 5 servings/week
Wine — 1 glass/day*
Olive oil – Regular use on food
The MIND diet limits servings of red meat, sweets, cheese, butter/margarine, and fast/fried food.
*Be careful about how much alcohol one drinks and how the body handles alcohol can change with age.
Dietary Supplements
Despite early findings of possible benefits for brain health, the research is inconclusive to prove that vitamin or supplement has been proven to work in people. Overall, evidence is promising, and much new research has been conducting to further prove the relationship. One such trial is happening in 2021. You can read more about the trial at High-Dose Vitamin D Supplements in Older Adults (alzheimers.gov).
Following few vitamins have been identified as potential drivel of the onset of Alzheimer; however, these studies are few or conducted on small population size and may need further research. In any case, identifying your vitamin deficiency and supplementing it with nutraceutical may not harm as long as it is taken as per the suggestion of the Primary Care provider. If taken properly, this could reduce the progression of Alzheimer’s disease.
Vitamin B
The B vitamins are a group of eight micronutrients that serve as coenzymes in many important biological processes. The specific B vitamins B2, B6, B12, and folate are involved in recycling the amino acid homocysteine during the cyclic generation of the amino acid methionine. Deficiencies in the amounts of these B vitamins can lead to increases in plasma homocysteine levels Homocysteine facilitates the generation of reactive oxygen species (ROS), promotes oxidative stress, and increases inflammation. High levels of homocysteine are one of the risk factors for AD. Vitamins B2, B6, and B12 decrease the level of homocysteine, thus helping to control Alzheimer’s Disease
Vitamin C
It is well established that individuals with mild cognitive impairment and Alzheimer’s disease have decreased plasma levels of ascorbic acid. Vitamin C, or ascorbic acid, is theorized to hamper Alzheimer’s disease.
Vitamin D
Vitamin D is linked to Alzheimer’s disease through regulation of calcium homeostasis, Aβ deposition, antioxidant, and anti-inflammatory properties. In animal studies, researchers have demonstrated improved cognitive function and reduced amyloid burden in response to vitamin D supplementation. The results from a large population-based study indicate that vitamin D intake in women with vitamin D deficiency show a lower cognitive decline compared to the control group
Vitamin D clearly has a beneficial role in Alzheimer’s disease and improved cognitive function in some patients. Genetic studies have provided the opportunity to determine what proteins link vitamin D to Alzheimer’s disease pathology. Vitamin D also exerts its effect on Alzheimer’s disease through nongenomic mechanisms. It is necessary to check the vitamin D status in patients with AD. Calcitriol is best used for Alzheimer’s disease because of its active form of vitamin D3 metabolite, and its receptor in the CNS.
Vitamin K
Evidence shows that individuals with Alzheimer’s disease often have low serum concentrations of vitamin K. Furthermore, geriatric patients that use vitamin K antagonists as anticoagulant medications suffer more frequent cognitive impairment. Vitamin K is involved in neuron development and survival through anti-apoptotic and anti-inflammatory effects. Vitamin K may decrease Alzheimer’s disease risk by modulating sphingolipid metabolism
BALANCE OF OMEGA-3/OMEGA-6 FATTY ACIDS
The imbalance of omega-3/omega-6 fatty acids in the typical Western diet sparks harmful peripheral inflammatory processes. Evidence suggests that the actions of omega-3 promote an anti-inflammatory state, while the actions of omega-6 increase inflammation. Increased ingestion of omega-6 fatty acid leads to the overproduction of omega-6 derived signaling molecules (eicosanoids), which when produced in large amounts appear to contribute to the onset of an inflammatory state through a variety of mechanisms, including the release of pro-inflammatory cytokines. Furthermore, increased omega-6 in the human diet coincides with the rising prevalence of obesity, a significant risk factor for Alzheimer’s disease development and progression that leads to widespread, systemic inflammation. A systematic review of 13 animal studies and 14 human studies supports the association between dietary omega-3/omega-6 fatty acids and the risk of developing Alzheimer’s disease. The evidence supports the role of omega-3 as anti-inflammatory fatty acid in preventing cognitive decline in Alzheimer’s disease at the early stage of the disease.
Medication
Recently US FDA approved Aduhelm (aducanumab) to treat patients with Alzheimer’s disease. Talk to your health care provider to learn more about the Medication.
Conclusion
- Getting checked by your primary care provider can help determine if the symptoms are related to Alzheimer’s disease, or a more treatable conditions such as a vitamin deficiency.
- Early and accurate diagnosis also provides opportunities for you and your family to slow down the progression of the disease, planning for future, and treatment options.
- There is promising evidence that focusing on Diet, Exercise and Supplements may slow down the progression of the Alzheimer’s disease.
If you are feeling symptoms and not satisfied with your current physician, we can help. Reach out to use for Second Medical option on your symptoms and our experts at KareOptions will be willing to help diagnose your condition and answer your questions.
Disclaimer:
“KareOptions does not have any intention to provide specific medical advice, but rather to provide its users and/ or the general public with information to better understand their health. All content (including text, graphics, images, information, etc.) provided herein is for general informational purposes only and is not a substitute for professional medical advice, care, diagnosis, or treatment. KareOptions makes no representation and assumes no responsibility/ liability for the accuracy of the information, advice, diagnosis, treatment provided herein or on its website. NEVER DISREGARD PROFESSIONAL MEDICAL ADVICE OR DELAY IN SEEKING TREATMENT BECAUSE OF SOMETHING YOU HAVE READ IT HERE OR ACCESSED THROUGH THE KAREOPTIONS WEBSITE.


