Introduction
Breast cancer is defined as the disease in which cancer develops inside the breast tissue. The disease is only second to skin cancer amongst women in the US. The awareness about breast cancer and funding of research has helped in creating advancement in the early detection and management of breast cancer. The survival rates are improving mainly due to an early screening of the disease, better treatment options, and understanding of the disease. The blog highlights various aspects of the disease like prevalence with the help of figures, symptoms, causes, screening methods, risk factors, preventive measures, and the latest medical advancement in the disease.
Facts and Figures
As per the latest figures released by the International Agency for Research on Cancer in Dec 2020, breast cancer is the leading most typical type of cancer detected and has overtaken lung cancer. The COVID-19 pandemic has worsened the situation due to late diagnosis of the disease due to lockdown restrictions and badly hit the low and middle socio-income nations. Moreover, cancer patients are at an increased risk of developing the symptoms of the Coronavirus due to more susceptibility to infections due to poor immunity.
Breast cancer is one of the most prevalent cancers in the US and around 281,500 new incidents were reported by the year 2021. The commonest symptom of the disease is the presence of a lump in the breast or armpit, alteration in shape and size of mammary glands, discharge from nipples, and red peeling skin. The commonest risk factor of the disease is genetic predisposition, overweight, alcohol intake, hormonal therapy, and age factor. In 2019, the 10-year probability of having breast cancer in the women belonging to the age group 20years was 0.1% whereas 4.1% in 70 years of age. In the year it was found that there were approximately 74,800 incidents of invasive breast cancer in the 60-69 age groups.
The management of the disease depends largely on the type and the stage of the disease. The commonest treatment options are surgical procedures, chemotherapy, radiation, and hormone replacement procedures. The initial stages of the disease are successfully corrected by breast-conservation surgery and radiation. The best part is that the survival rates are pretty high and around 90% of women survive five years past their diagnosis. Survival rates become better by early screening and detection of the disease. The US Preventative Services Taskforce suggests that there must be a compulsory mammogram in two years for women in the age group 50-74 years. In 2018, the number of patients who received a mammogram in 2 years was around 67% with government-based insurance services and around 77% with private insurance.
Symptoms
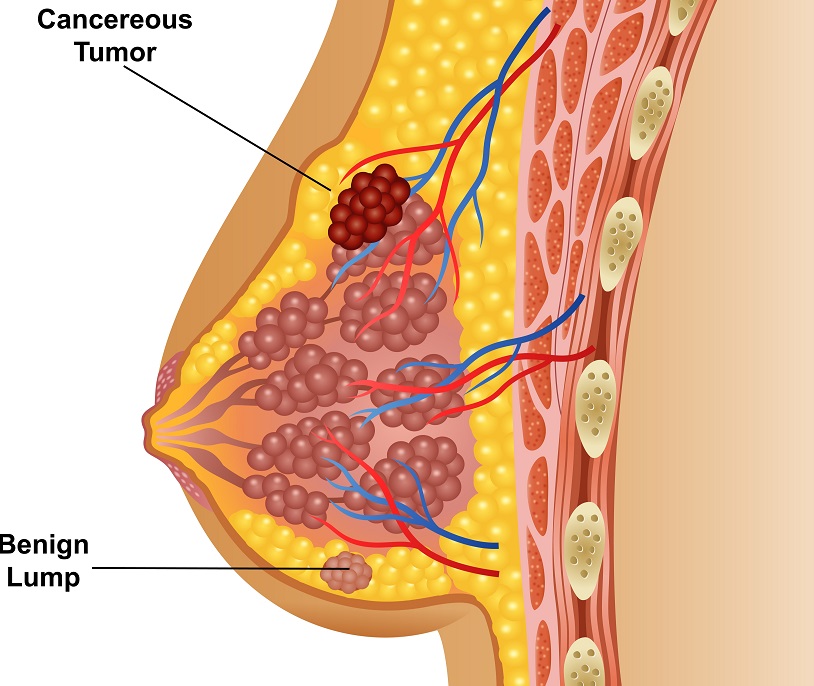
- Presence of lump in the breast or armpit
- Alteration in shape and size of mammary glands
- Discharge from nipples
- Peeling, scaling, and crusting of skin around nipples
- Alterations in the skin of the breast like dimpling
- Presence of newly discovered inverted nipples
- Pitting of the skin of the breast
Causes
The researchers have found that the condition of breast cancer develops when the cells inside the breast tissue begin to grow uncontrollably and accumulate to form a lump. These cells may move to different places like axillary lymph nodes or other parts of the body. The most common area where excessive multiplication takes place is milk-producing ducts although the disease may initiate from the lobules or the glandular tissue (Mayo Clinic, n.d.). Extensive research on the disease helped to find out that hormonal imbalance, lifestyle changes, and environmental factors are the contributing factors to breast cancer. However, it can not be explained that why some high-risk remain unaffected while the low-risk people develop the disease. This can be explained by the fact that the illness precipitates due to the complicated interaction of the genome of an individual with the environment.
Screeing
The screening of the disease means examining a woman’s breast even before the development of any signs or symptoms of the disease. This is not a curative measure but helps in the early detection of the disease and better prognosis. USPTF is an institution comprising doctors and experts who conduct research on the disease and offer advice about early detection of the disease. The institution has suggested that women belonging to 50-74 years must undergo a mammogram once in 2 years while women in the age group 40-49 years must consult the doctor regarding screening options.
- Mammogram: it is a diagnostics test for the detection of breast cancer and is an X-ray of the breast.
- Breast MRI: this procedure utilizes magnet and radio waves to take images of the breast and it is often done along with a mammogram to confirm the diagnosis of the disease.
- Clinical examination: is performed by a doctor to check the presence of any lump or any other abnormalities in the breast.
- Self-examination: regular self-monitoring of breasts for the presence of lumps
Risk Factors
The presence of risk factors increases the probability of developing the disease. However, it has been observed that people without having any risk factors develop the disease while the ones with multiple risk factors are free from breast cancer.
- Age: older age increases the risk of developing the disease.
- Previous history of breast-related issues: like lobular carcinoma in situ or atypical hyperplasia of breast tissue then the chances of developing the disease increases and also the history of carcinoma of one breast increases the risk of developing the disease in the remaining one.
- Family history
- Inherited gene mutations: some gene mutations like BRCA1 and BRCA2 enhances the risk of developing breast and other types of cancers.
- Exposure to harmful radiation.
- Obese women are at greater risk of developing the disease.
- Early menarche also increases the probability of culminating the disease at later stages
- Late menopause also increases the risk of developing the disease.
- If the first child is born when the female is over 30 years then the chances are higher to have the disease.
- Women who have never been pregnant are also at increased risk.
- Post-menopausal hormone replacement therapy like a combination of estrogen and progesterone is at an increased risk.
- Alcohol consumption also increases the risk of developing cancer.
Preventive Measures
On the brighter side, it is pertinent to highlight that the risk of developing breast cancer can be minimized by following a range of measures:
- Women should make it a routine to go for regular checkups and screening which includes breast exams and mammograms. The physician can help decide the right diagnostic tool as per the different backgrounds of the patients.
- Besides consulting the doctor, a habit of self-examination should be inculcated. In case of any changes, lumps, or lesions, immediate medical advice should be sought. Such an examination helps women accept the normal hormonal changes that reflect in the breast region and the unusual ones which require medical supervision (Tsvetkova, 2019).
- Women should limit their alcohol consumption or avoid it altogether.
- Maintaining physical fitness can help get rid of toxins and adopt a healthy routine. The target for at least 30 minutes of physical activity should be maintained after consulting with the doctor.
- Constraining hormone therapy post-menopause can also reduce the incidence of breast cancer. The potential pros and cons of hormone therapy should be discussed with the doctor. Empirical evidence suggests that some women notice severe symptoms in the post-menopause phase, for which hormone therapy may be recommended. However, a minimal dosage of this therapy should be taken.
- Try to maintain a healthy weight by considering your Body Mass Index. If weight loss is required, consult your doctor before hitting the gym or opting for intermittent fasting. A mix of healthy strategies should be adopted to get rid of fat. The rate of calories burned should be slow and sustainable.
- A healthy diet is the key to a healthy body. As per various reports, it is highlighted that the Mediterranean diet cooked using extra virgin olive oil and dried fruits reduces the risk of breast cancer. Make sure to include plant-based foods in your diets such as legumes, almonds, wholesome grains, fruits, and vegetables. Try to substitute olive oil for butter and fish for meat.
Management
Breast cancer begins its course when certain cells in the region begin to expand abnormally. The division of cells gets rapid as compared to the healthy cells in the body and unhealthy cells accumulate to form a lump or mass. At a later stage, cells begin to metastasize via lymph nodes affecting other parts of the body. However, the initial outbreak of the disease often takes place in the ducts that produce milk often termed invasive ductal carcinoma. In certain cases, it may start in the glandular tissues known as lobules which are termed invasive lobular carcinoma. There is a wide range of determinants that put women at risk of breast cancer. The most prominent amongst them include lifestyle, hormonal or environmental causes. A complex or unlikely interplay between your genes and external environment can also lead to the spurring of the deadly disease (Tong et al., 2018).
The high-risk women can resort to chemo-prevention medications that essentially involve estrogen blockages such as estrogen modulators or aromatase inhibitors. But these preventive measures do bring along various side effects and are often restrained by doctors. Another option available for high-risk women is a prophylactic mastectomy, a procedure that involves the amputation of healthy breasts. Prophylactic oophorectomy is also an alternative for women who want to significantly reduce the risk of both breast and ovarian cancer.
Medical advancements in the field of breast cancer are a new ray of hope in the patients. These techniques have helped to increase the survival rates and lower the mortality rates.
HER2 therapy human epidermal growth factor receptor 2 is a protein that increases the growth of cancer cells. This treatment plan can be effectively used in the early and late stages of cancer. But not all patients show overexpression of these proteins. The drugs include Herceptin, lapatinib, and pertuzumab
Gene expression examination: these are the tests to identify the type of genes that expresses cancer. This method helps to understand which management option will be effective for the patient whether chemotherapy or hormone replacement therapy.
Hormonal replacement therapy these procedures assist in preventing the binding of estrogen to the estrogen receptor-positive disease. The blockage of the synthesis of estrogen helps in the treatment of cancer (Cancer Research Institute, 2018).
Less invasive surgery: To understand the spread of the disease lymph nodes are removed and assessed. Patients with no sentinel node cancer may not need to go for advanced surgical procedures. Exercise and a Healthy Lifestyle: The maintenance of a healthy weight prevents the recurrence of the disease (Vorobiof, 2016).
Questions to Ask the Health Care Team
Having a detailed discussion with your healthcare team helps you take an informed decision on your treatment plan and diagnosis. Here’s a list of questions you should ask your healthcare team after getting a diagnosis.
- Is there enough information to recommend a treatment plan for me? If not, which tests or procedures will be needed? Will I need to see other doctors?
- What are my treatment plan options?
- What treatment plan do you recommend? Why?
- Whom would you recommend for a second opinion?
- When do I need to make a treatment decision?
- Who will be part of my health care team, and what does each member do?
- Who will lead my overall treatment?
- What is the goal of each treatment? Is it to eliminate cancer, help me feel better, or both?
- What can I do to get ready for treatment?
- If I am worried about managing the costs of cancer care, who can help me? Who can help me understand what aspects of my care are covered by my insurance?
- If I have questions or problems, who should I call?
- Do you communicate with your patients by email or with an electronic health record system?
- If have a strong family history of cancer, what is my chance of getting another cancer? How does that change my treatment options? Should I see a genetic counselor?
- Do you have a social worker I can speak with?
- What should I tell my employer, if anything, and what laws protect my rights as an employee?
How Can KareOptions Help you Get a Second Opinion?
Finding the right doctor for getting a second opinion and dealing with insurance concerns may be overwhelming for most patients. Some patients may even feel awkward telling their current doctor that they would like a second opinion. Sometimes, your doctor may be able to help you find the right specialist, but in most cases, you have to do a lot of work finding the right doctor without delaying your essential treatment. Insurance companies may or may cover the cost of a second opinion, and some may reimburse your costs when you consult a specialist who belongs to their approved lists of providers.
KareOptions can simplify the process of getting a second opinion for your cancer treatment by undertaking all the groundwork to get access to specialists that suit your healthcare needs. Our Medical Second Opinion Service (MSOS) and Second Opinion Board Review (SOBR) help you obtain a sound review of your diagnosis and treatment options by a team of oncology experts.
Related Blogs:
Should you get a Second Opinion on your Breast Cancer Diagnosis
Understanding Cancer- Awareness about cancer is already the half battle won
How Can a Second Opinion Guide you in Understanding Side Effects of your Cancer Treatment
How can cancer experts guide you in coping with the disease
How to prepare yourself before getting a second medical opinion?
Disclaimer:
“KareOptions does not have any intention to provide specific medical advice, but rather to provide its users and/ or the general public with information to better understand their health. All content (including text, graphics, images, information, etc.) provided herein is for general informational purposes only and is not a substitute for professional medical advice, care, diagnosis, or treatment. KareOptions makes no representation and assumes no responsibility/ liability for the accuracy of the information, advice, diagnosis, treatment provided herein or on its website. NEVER DISREGARD PROFESSIONAL MEDICAL ADVICE OR DELAY IN SEEKING TREATMENT BECAUSE OF SOMETHING YOU HAVE READ IT HERE OR ACCESSED THROUGH THE KAREOPTIONS WEBSITE.


